Going Viral: Ebola and Viral Haemorrhagic Fevers as Bioweapons
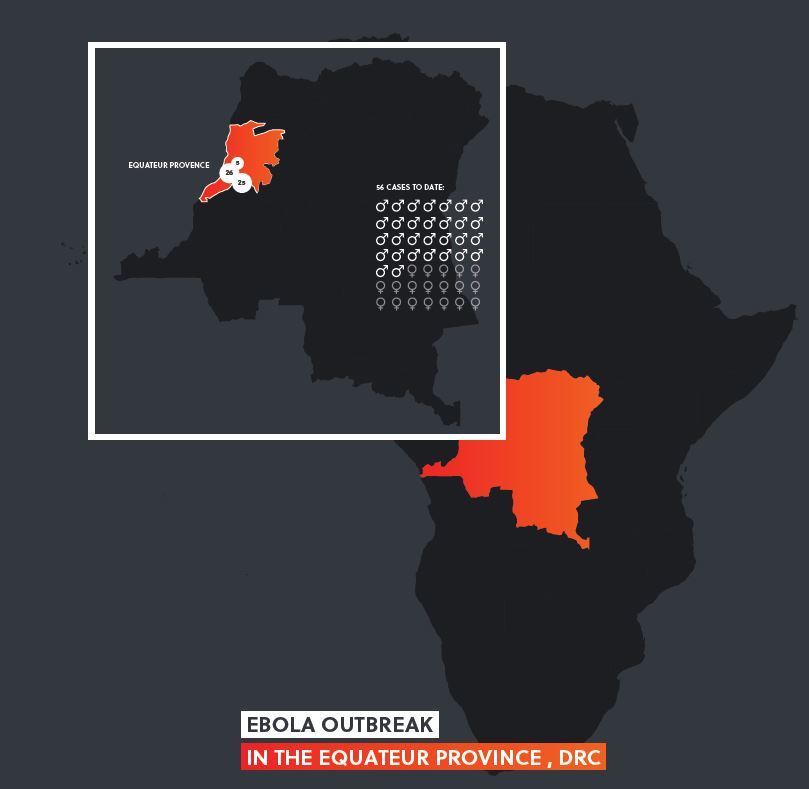
The 2014 West African outbreak of Ebola, affecting Guinea, Liberia, and Sierra Leone, led to the infection of an estimated 23,000 people, and the deaths of an estimated 11,000 people. This outbreak, the largest recorded incident in modern history, and infected approximately 11 times the number of all previous combined Ebola outbreaks. The current outbreak in the Democratic Republic of Congo, in which 21 people have died (as of 21 May 2018), has renewed fears of a large-scale outbreak. However, the early deployment of the unlicensed Ebola vaccine will likely mitigate the spread of the disease.
The aforementioned large-scale outbreak of Ebola, in addition to Hollywood’s references to VHFs in popular mainstream pandemic-themed films, has captured the public imagination and fuelled fears surrounding the use of Ebola as a biological weapon. These concerns have increased, despite the fact that in a developed country with a robust healthcare system, patients would be rapidly isolated and preventative measures implemented.
The most significant effect of a weaponised Ebola virus is less likely to be the body-count, than the fear that surrounds the disease. As the mass-hysteria caused by a bio-weapon spreads, it may affect not only the general public, but also those who would typically respond and protect societal stability in the event of an outbreak, such as healthcare workers, security personnel and policy-makers. To quote Anthony Fauci, the head of the National Institute of Allergy and Infectious Diseases; “when talking about bioterror, it’s more about the terror than it is the bio”.

PREVIOUS ATTEMPTS AT WEAPONISATION
While no state has yet succeeded in weaponising Ebola, many have tried. Most notable among those is the former Soviet Union, which began its biological weapons programme in the 1920s, and continued developing offensive capabilities into the 1990s. According to Ken Alibek, a former Soviet biological warfare expert, and current US-based bio-weapons consultant, the Soviet bio-weapons program attempted to weaponise Ebola and other VHFs, although the final state of the program’s progress remains unclear. Alibek claims that the Soviet program had succeeded in developing a VHF as a weapon, but no evidence exists to corroborate these claims. It is widely believed in the scientific and intelligence communities that the Soviet programme generally focused on biological agents that were easier to produce, such as anthrax.
In fact, the only realistic scenario for the development of a weaponised VHF would be a state-sponsored biological warfare programme. The development of these classes of viruses for weaponisation requires advanced technical knowledge, as well as plenty of time and patience, as viruses are notoriously difficult to culture, even in a laboratory environment. Furthermore, the technological requirements to safely produce enough virus to be an effective weapon requires a Biosafety Level-4 laboratory, with the highest level of safety procedures, of which there are only 50 worldwide.
The only realistic scenario for the development of a weaponised VHF would be a state-sponsored biological warfare programme.
EBOLA AND TERRORISM
Based on the high morbidity and mortality, historical investigations and socioeconomic impact, Ebola is classified as a “Category A Bioterrorism Agent” by the US Centers for Disease Control and Prevention. Publically, fears of militant groups obtaining, creating and utilising weaponised Ebola have also been debated in policy-making circles, academia and public forums. For example, in 2003, a panel of experts investigated the potential of a terrorist attack using VHFs as biological weapons.
The most significant concern facing states is that a terrorist organisation could obtain samples of Ebola and develop a biological weapon. There are two potential scenarios in which a terrorist group could obtain samples of Ebola:
- Theft. The primary fear is that a terrorist group gains access to a BSL-4 laboratory where scientists are studying Ebola. However, the security procedures of many BSL-4 laboratories are confidential, and the likelihood of such a plan succeeding is low. Based on existing public knowledge of BSL-3 facilities, if an individual could gain access, they are unlikely to be able to identify the agent, or its location, without insider knowledge. Most samples in such laboratories are stored in a pseudo-anonymised manner, with only the relevant researchers having an exact knowledge of the contents of a sample.
- Direct collection. Another scenario is that a terrorist group could travel to an area where there is an ongoing outbreak and retrieve a sample directly from an infected source. However, the risks associated with obtaining a sample are significant, and are generally undertaken by healthcare professionals with specialised training to prevent the infection of the person obtaining the sample. Samples are also tightly controlled in outbreaks, to prevent the spread of the disease, and theft would likely be incredibly difficult. Furthermore, given the facilities needed to develop the weapon after accessing a sample, this a scenario is significantly decreased by the low likelihood that terrorist organisations would have the resources, know-how or operational capabilities to create a bio-weapon in the first place.
THE ECONOMIC AND HEALTHCARE IMPACT OF AN EBOLA OUTBREAK
Over the course of 2015, the economic impact of the 2014 outbreak was a USD 2.2 billion combined loss in GDP in Guinea, Liberia, and Sierra Leone. The impact was partially due to a substantial loss in private sector growth, declining agricultural production, and a decrease in cross-border trade. Restrictions on movement, goods and services were increased, in an attempt to prevent the spread of Ebola. According to the US Centers for Disease Control and Prevention (CDC), Sierra Leone lost approximately half its private sector work force.
While the economic impact of the 2014 Ebola outbreak was immense, the devastating effects on the local and international healthcare community were equally significant, as healthcare workers treating patients are at greater risk for contracting the disease. In the 2014 outbreak in West Africa, 881 healthcare providers contracted the disease, and 513 died as a result. In Sierra Leone alone, the impact on healthcare workers led to an 8 percent reduction in the healthcare workforce, and a 23 percent decrease in health services delivery in the country. The indirect impact of the outbreak on the healthcare industry in Guinea, Liberia, and Sierra Leone led to an estimated 10,600 additional deaths due to other diseases, as there were simply fewer healthcare workers available to treat patients suffering from non-Ebola illnesses.